Testosterone (Pre-menopausal)
Testosterone is an androgen made in smaller amounts by the ovaries and adrenal glands in pre-menopausal women. On this panel it’s measured in urine and typically reported normalized to creatinine (e.g., µg/g creatinine) so hydration doesn’t skew results. Urinary testosterone reflects how much testosterone your body produces and clears over time and should be interpreted alongside other hormones (EPI-testosterone, DHEA(-S), androstenedione, SHBG on serum, and 5-α/5-β metabolites where available). Because it’s urine—not blood—this marker is best for pattern-finding and trending, not for making a diagnosis by itself.
Why testosterone matters in pre-menopausal women
-
Supports energy, mood, motivation, and sexual desire.
-
Helps maintain lean muscle, bone, and metabolic health.
-
Imbalances (too low or too high for you) can contribute to symptoms such as fatigue, low libido, irregular cycles, acne, hirsutism (chin/upper-lip hair), or scalp hair thinning—but symptoms depend on the whole hormone picture, not testosterone alone.
How to read your result (always use your lab’s reference range)
-
In range (typical): Consistent with balanced androgen output for a pre-menopausal woman. Correlate with how you feel and with companion markers.
-
Low: May be seen with hormonal contraception, hypothalamic amenorrhea/low energy availability, chronic illness, post-partum, some antidepressants, glucocorticoids, or after oophorectomy. Symptoms can include low libido, reduced exercise capacity, low mood, and brain fog—but confirm with serum tests (total/free testosterone, SHBG) and clinical context before labeling it “deficiency.”
-
Elevated: Can occur with polycystic ovary syndrome (PCOS), insulin resistance, non-classic congenital adrenal hyperplasia (NCCAH; 21-hydroxylase), adrenal/ovarian androgen excess, or rarely androgen-secreting tumors. Often pairs with low SHBG (on serum), high androstenedione or DHEA-S, and clinical signs (acne, hirsutism, cycle irregularity). Urine results alone do not diagnose these conditions—use them to guide targeted follow-up.
Factors that can shift urine testosterone
-
Cycle phase: Levels can vary slightly across the cycle; many labs prefer follicular timing for comparison.
-
Medications & hormones: Oral contraceptives, progestins, anti-androgens (spironolactone, finasteride), glucocorticoids, or testosterone therapy change patterns.
-
Metabolic status: Insulin resistance, obesity, very low-carb or very low-calorie diets, and overtraining can all nudge androgens.
-
Alcohol/sleep/stress: Short-term changes are possible; aim for a typical day before collection.
-
Collection issues: Non–first-morning samples, very dilute urine, or heavy fluid intake can push borderline values; creatinine correction helps but isn’t perfect.
Symptoms & clinical clues to consider with an out-of-range result
-
Low-leaning pattern: Low libido, low energy, difficulty building muscle, low mood, bone-health concerns (especially if estradiol is also low).
-
High-leaning pattern: Acne, hirsutism, scalp hair thinning, irregular/absent periods, weight gain around the middle, or A1C/insulin creeping up.
-
Red flags (urgent eval): Rapid-onset virilization (voice deepening, clitoromegaly), very high androgen levels, or sudden, severe symptoms—seek prompt specialist care.
What to do next (actionable plan)
If low or borderline low:
-
Repeat under ideal conditions (first-morning urine, typical sleep/food, no heavy alcohol the night before).
-
Discuss serum testing: total testosterone, free testosterone (or calculated free using SHBG and albumin), SHBG, and estradiol.
-
Address foundations: adequate protein, resistance training, sleep, stress management; review meds (e.g., OCPs, SSRIs, steroids).
-
Consider endocrinology/gynecology input if symptoms are significant.
If elevated or borderline high:
-
Confirm with a repeat and ensure proper timing/collection.
-
Order targeted labs with your clinician: serum total & free testosterone, SHBG, DHEA-S, androstenedione, LH/FSH, 17-hydroxyprogesterone (AM, follicular), TSH, prolactin, plus A1C/fasting insulin when insulin resistance is suspected.
-
If PCOS is likely: evaluate ovulation patterns, ovarian ultrasound (when appropriate), and metabolic risk.
-
If very high or rapidly rising: urgent endocrinology/gynecology referral and imaging to exclude rare androgen-secreting tumors.
-
Interventions focus on the cause (e.g., lifestyle and insulin sensitization for PCOS/IR; specific therapy for NCCAH; medication review).
How this marker fits with the rest of your panel
-
Pair with EPI-Testosterone (epitestosterone) to understand the broader androgen landscape (EPI-T has weak antiandrogen activity and is relatively unaffected by exogenous testosterone).
-
Review DHEA-S and androstenedione (adrenal/ovarian precursors).
-
Consider 5-α-reduced metabolites (e.g., androsterone) if available to gauge conversion toward DHT activity.
-
Always integrate serum SHBG to understand free/bioavailable androgen exposure at tissues.
Key takeaways
-
Urinary testosterone helps you and your clinician see your androgen pattern over time but shouldn’t be used alone for diagnosis.
-
Low values can reflect contraception, low energy availability, or HPO-axis suppression; high values suggest androgen excess states like PCOS or NCCAH—confirm with serum tests and clinical assessment.
-
Optimize collection, repeat if borderline, and treat the root cause, not just the number.
Lab Results Explained and Tracked
What does it mean if your Testosterone (Pre-menopausal) result is too high?
An elevated urinary testosterone suggests your body is producing and/or clearing more androgen than expected for a pre-menopausal woman. Because this is a urine test (a reflection of output over time), it’s most useful for pattern-finding and trending. An isolated high value does not diagnose any condition by itself—interpret it with your symptoms and with companion markers (EPI-testosterone, DHEA-S, androstenedione, 5-α/5-β metabolites, and, on serum, SHBG and free testosterone).
Common reasons testosterone can be high
-
Polycystic Ovary Syndrome (PCOS) or insulin resistance/metabolic syndrome (very common): may coexist with irregular/absent ovulation, acne, hirsutism, scalp hair thinning, weight gain around the middle, and low SHBG on serum.
-
Adrenal-driven androgen excess: e.g., non-classic congenital adrenal hyperplasia (NCCAH; 21-hydroxylase) or chronic ACTH drive; often accompanied by elevated 17-hydroxyprogesterone (serum).
-
Ovarian sources: functional ovarian hyperandrogenism/hyperthecosis; rarely, an androgen-secreting ovarian tumor (usually very high and rapidly progressive).
-
Medications/supplements: exogenous testosterone, certain prohormones, high-dose DHEA, or drugs that alter steroid metabolism.
-
Physiologic/collection factors: cycle timing differences, very dilute urine, non–first-morning collection, major stress/sleep loss, or heavy training right before sampling can nudge borderline results.
Symptoms and clinical clues that fit a “high-androgen” picture
-
Skin/hair: Acne, increased facial/body hair (hirsutism), scalp hair thinning.
-
Cycles: Irregular or absent periods, signs of anovulation.
-
Metabolic: Central weight gain, elevated fasting insulin/A1C, dyslipidemia.
-
Red flags (seek prompt evaluation): Rapid-onset virilization (voice deepening, clitoromegaly), very fast progression of symptoms, or very high androgen levels.
How to read your number
-
Borderline/slightly above range: Often due to timing, hydration, or day-to-day variability. Repeat with a first-morning sample, ideally in the early follicular phase (cycle days ~3–10) if your lab recommends it.
-
Clearly/persistently elevated: More likely reflects a true androgen excess state—interpret with the pattern of other urine and serum hormones and your clinical picture.
What to do next (practical plan)
-
Confirm correctly
-
Repeat using a first-morning urine sample; follow collection instructions; avoid unusually high fluid intake, all-nighters, and heavy training the day before. Note cycle day and any hormones/meds.
-
-
Add targeted serum testing (with your clinician)
-
Total & free testosterone (or calculated free using SHBG and albumin), SHBG, DHEA-S, androstenedione, LH/FSH, 17-hydroxyprogesterone (AM, follicular), TSH, prolactin; consider A1C/fasting insulin if insulin resistance is suspected.
-
-
Address likely causes
-
PCOS/insulin resistance: nutrition quality, resistance training, sleep, stress, weight management; discuss insulin-sensitizing strategies with your clinician.
-
NCCAH or adrenal causes: endocrine evaluation; specific therapy if confirmed.
-
Medication/supplement review: reassess exogenous androgens, DHEA, or other agents that raise androgens.
-
-
Escalate when appropriate
-
Very high or rapidly rising levels, or virilizing symptoms → urgent endocrinology/gynecology referral and targeted imaging to exclude rare tumors.
-
Related markers to review together
-
EPI-Testosterone (epitestosterone): context marker; weak antiandrogen.
-
DHEA-S & androstenedione: adrenal/ovarian precursors that help localize the source.
-
5-α-reduced metabolites (e.g., androsterone, 5-α-androstanediol): indicate conversion toward DHT activity.
-
Serum SHBG: essential for estimating free/bioavailable androgen exposure at tissues.
Key takeaways
-
Elevated urinary testosterone signals higher androgen output/clearance, but urine alone isn’t diagnostic.
-
The pattern across urine and serum markers—plus your symptoms—guides next steps.
-
Confirm properly, identify the root cause (PCOS/IR, adrenal, ovarian, medication), and tailor treatment with your clinician.
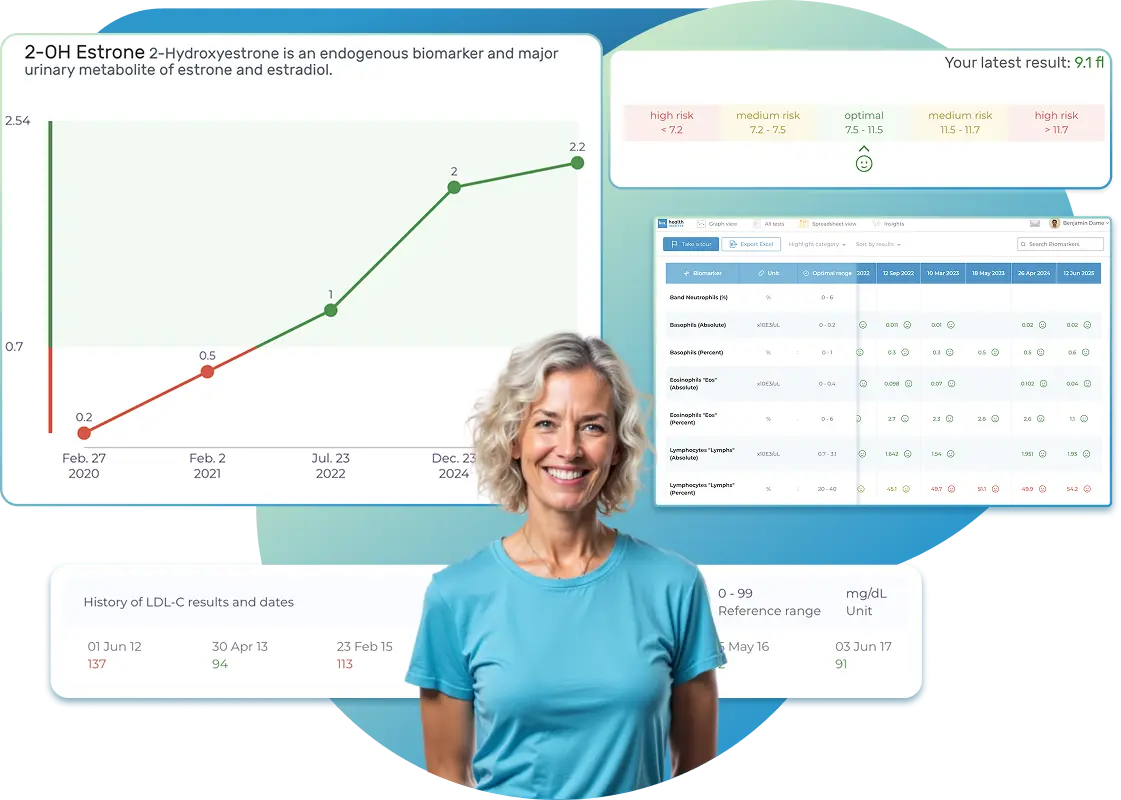
All Your Lab Results.
One Simple Dashboard.
Import, Track, and Share Your Lab Results Easily
Import, Track, and Share Your Lab Results
Import lab results from multiple providers, track changes over time, customize your reference ranges, and get clear explanations for each result. Everything is stored securely, exportable in one organized file, and shareable with your doctor—or anyone you choose.
Cancel or upgrade anytime
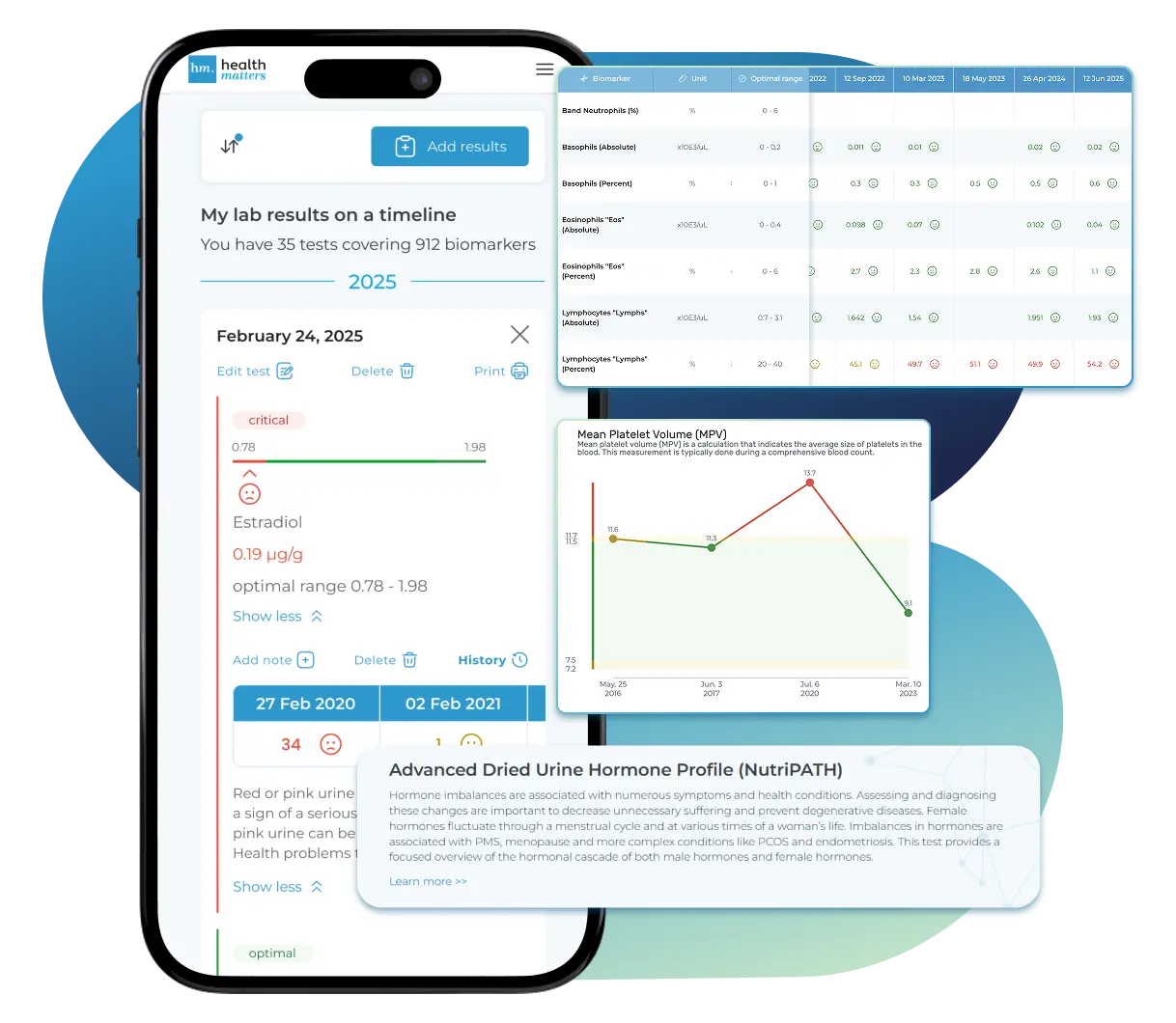
What does it mean if your Testosterone (Pre-menopausal) result is too low?
Low urinary testosterone levels in women can be a sign of several underlying issues, including:
- Adrenal insufficiency: The adrenal glands are a key source of testosterone in women. Dysfunction may result in low levels.
- Chronic stress and high cortisol: Chronic stress suppresses hormone production, leading to hormonal imbalances.
- Hypothalamic-pituitary dysfunction: Reduced signaling from the brain can impair hormone production.
- Age-related decline: Testosterone naturally declines with age, particularly during menopause.
- Ovarian insufficiency or dysfunction: Conditions like premature ovarian failure can reduce hormone levels.
- Nutritional deficiencies: Low zinc, vitamin D, or other nutrients necessary for hormone production may lead to low testosterone.
- Estrogen dominance: Excess estrogen can suppress testosterone levels, creating an imbalance.
Symptoms of Low Testosterone in Women
- Fatigue and low energy
- Loss of muscle mass and decreased strength
- Low libido or sexual dysfunction
- Mood changes (depression, irritability, or anxiety)
- Weight gain, particularly around the midsection
- Thinning hair or hair loss
- Decreased bone density (osteopenia or osteoporosis)
Treatment Options for Low Testosterone
-
Lifestyle and Nutritional Changes
- Manage stress: Practices like meditation, yoga, and adequate sleep help balance cortisol levels.
- Exercise: Resistance training and high-intensity interval training (HIIT) can boost testosterone.
- Optimize diet: Include healthy fats, lean proteins, and nutrient-rich foods. Focus on zinc, magnesium, and vitamin D.
- Weight management: Maintaining a healthy body weight supports hormone balance.
-
Supplementation
- DHEA (Dehydroepiandrosterone): Precursor to testosterone, often used to boost androgen levels.
- Zinc, Vitamin D, and Magnesium: Support testosterone production.
- Adaptogens (Ashwagandha, Maca): Help balance cortisol and improve adrenal function.
-
Hormone Replacement Therapy (HRT)
- Bioidentical testosterone therapy: Low doses of testosterone can be prescribed to restore levels.
- Combination therapy: Often combined with estrogen or DHEA to achieve optimal balance.
- This should be carefully monitored by a healthcare provider to avoid side effects like acne, hair growth, or mood swings.
-
Addressing Underlying Conditions
- Treat adrenal insufficiency, thyroid disorders, or PCOS if they contribute to low testosterone.
Why Balancing Testosterone Is Important
Restoring healthy testosterone levels can improve overall well-being by enhancing mood, energy, libido, and muscle strength. It also reduces the risk of osteoporosis and promotes long-term cardiovascular and metabolic health.
Article Review & Sources
All our content is backed by peer-reviewed studies, academic research, and trusted medical sources. We're committed to accuracy and transparency — see our editorial policy for details.
Laboratories
Bring All Your Lab Results Together — In One Place
We accept reports from any lab, so you can easily collect and organize all your health information in one secure spot.
Pricing Table
Gather Your Lab History — and Finally Make Sense of It
Finally, Your Lab Results Organized and Clear
Personal plans
$79/ year
Advanced Plan
Access your lab reports, explanations, and tracking tools.
- Import lab results from any provider
- Track all results with visual tools
- Customize your reference ranges
- Export your full lab history anytime
- Share results securely with anyone
- Receive 5 reports entered for you
- Cancel or upgrade anytime
$250/ once
Unlimited Account
Pay once, access everything—no monthly fees, no limits.
- Import lab results from any provider
- Track all results with visual tools
- Customize your reference ranges
- Export your full lab history anytime
- Share results securely with anyone
- Receive 10 reports entered for you
- No subscriptions. No extra fees.
$45/ month
Pro Monthly
Designed for professionals managing their clients' lab reports
- Import lab results from any provider
- Track lab results for multiple clients
- Customize reference ranges per client
- Export lab histories and reports
- Begin with first report entered by us
- Cancel or upgrade anytime
About membership
What's included in a Healthmatters membership
 Import Lab Results from Any Source
Import Lab Results from Any Source
 See Your Health Timeline
See Your Health Timeline
 Understand What Your Results Mean
Understand What Your Results Mean
 Visualize Your Results
Visualize Your Results
 Data Entry Service for Your Reports
Data Entry Service for Your Reports
 Securely Share With Anyone You Trust
Securely Share With Anyone You Trust
Let Your Lab Results Tell the Full Story
Once your results are in one place, see the bigger picture — track trends over time, compare data side by side, export your full history, and share securely with anyone you trust.





Bring all your results together to compare, track progress, export your history, and share securely.
What Healthmatters Members Are Saying
We implement proven measures to keep your data safe.
At HealthMatters, we're committed to maintaining the security and confidentiality of your personal information. We've put industry-leading security standards in place to help protect against the loss, misuse, or alteration of the information under our control. We use procedural, physical, and electronic security methods designed to prevent unauthorized people from getting access to this information. Our internal code of conduct adds additional privacy protection. All data is backed up multiple times a day and encrypted using SSL certificates. See our Privacy Policy for more details.

















