Choline is an essential nutrient that plays a foundational role in brain health, liver function, methylation, and neurotransmitter synthesis. It serves as both a structural building block for cell membranes and a biochemical precursor for several key molecules, including acetylcholine (a neurotransmitter critical for memory, focus, and muscle control) and betaine (trimethylglycine), a major methyl donor in the body.
On the Neurotransmitter XL panel, choline reflects the body’s capacity to maintain membrane integrity, neurotransmitter balance, and methylation efficiency. Adequate choline ensures optimal communication between neurons, healthy liver metabolism, and efficient detoxification through the methionine cycle, which depends on methyl donors for proper function.
Because the brain and liver are among the most metabolically active organs, choline status is often a key indicator of both cognitive performance and cellular energy balance.
Biochemical Role and Function
1. Precursor to Acetylcholine
Choline is converted into acetylcholine, one of the brain’s most important neurotransmitters, by the enzyme choline acetyltransferase. Acetylcholine governs attention, learning, memory, and muscle contraction. Low choline availability can directly limit acetylcholine synthesis, affecting mental sharpness, memory retention, and focus.
2. Structural Component of Cell Membranes
Choline contributes to the formation of phosphatidylcholine (PC) and sphingomyelin, key phospholipids that maintain cell membrane integrity and support neuronal communication. Phosphatidylcholine also plays a central role in lipid transport, helping prevent fat accumulation in the liver and promoting proper cell signaling and repair.
3. Methylation and Homocysteine Regulation
Through its oxidation into betaine, choline participates in methyl group donation—a vital process for DNA methylation, gene regulation, and neurotransmitter metabolism. Betaine donates methyl groups via the betaine-homocysteine methyltransferase (BHMT) pathway, which converts homocysteine into methionine, sustaining S-adenosylmethionine (SAM) production.
This connection makes choline essential for maintaining balanced homocysteine levels and efficient methylation alongside folate, vitamin B12, and vitamin B6.
4. Liver Function and Fat Metabolism
Choline is indispensable for liver health, as it supports the synthesis of phosphatidylcholine required for VLDL (very-low-density lipoprotein) export. Without enough choline, fat accumulates in the liver, leading to non-alcoholic fatty liver disease (NAFLD) and impaired detoxification.
5. Cellular Energy and Mitochondrial Protection
By promoting membrane fluidity and supporting methylation-dependent ATP synthesis, choline indirectly maintains mitochondrial efficiency and protects against oxidative stress.
Choline and the Nervous System
Within the nervous system, choline serves as a link between neurochemical communication and metabolic stability:
-
Acetylcholine production: Crucial for cognitive function, learning, and REM sleep regulation.
-
Methylation of neurotransmitters: Through betaine and SAM support, choline assists in dopamine, serotonin, and adrenaline metabolism.
-
Membrane composition: Phosphatidylcholine and sphingomyelin ensure optimal receptor sensitivity and signal transmission between neurons.
Deficiency in choline can manifest as mental fatigue, brain fog, irritability, or low focus, reflecting both neurotransmitter and membrane instability.
Causes of Low Choline Levels
1. Insufficient Dietary Intake
Choline is found primarily in animal-based foods such as eggs, fish, chicken, and liver. Plant-based diets, especially vegan or low-protein diets, may provide inadequate amounts. The body can synthesize small amounts of choline via the PEMT enzyme (phosphatidylethanolamine N-methyltransferase), but this pathway alone is insufficient to meet full metabolic demands.
2. Increased Methylation Demand
Chronic stress, toxin exposure, or inflammation increases the need for methyl donors, depleting choline stores faster than they can be replenished. This can occur even with normal dietary intake.
3. Genetic Variants (PEMT, BHMT, MTHFR)
-
PEMT polymorphisms reduce endogenous phosphatidylcholine synthesis.
-
BHMT and MTHFR variants can impair methylation efficiency, causing over-reliance on choline as a methyl donor.
These genetic factors increase susceptibility to low choline levels, especially when dietary intake or B-vitamin status is suboptimal.
4. B-Vitamin Deficiency
Because choline works closely with B12, folate, and B6 in the methylation cycle, deficiencies in these vitamins can reduce the efficiency of both homocysteine recycling and SAM regeneration, indirectly depleting choline reserves.
5. Liver or Gut Dysfunction
Poor liver function or bile flow impairs both choline synthesis and absorption. Gut inflammation or dysbiosis may further limit uptake and increase degradation, reducing systemic availability.
Symptoms of Low Choline Levels
Low choline levels can affect multiple systems, particularly the brain, liver, and methylation pathways. Common symptoms include:
Cognitive and Neurological Signs:
-
Brain fog, memory loss, or poor focus
-
Fatigue or lack of mental clarity
-
Difficulty concentrating or learning
-
Low mood or irritability
-
Muscle tension or weakness (due to low acetylcholine)
Metabolic and Systemic Signs:
-
Elevated homocysteine levels
-
Fatty liver or impaired fat metabolism
-
Digestive sluggishness or bloating
-
Poor detoxification (sensitivity to caffeine, alcohol, or medications)
-
Hormonal imbalance, particularly estrogen dominance in women
Choline deficiency may also worsen oxidative stress and mitochondrial strain, leading to symptoms of chronic fatigue or “wired-but-tired” energy patterns.
Interpretation Context on Neurotransmitter XL
| Related Marker | Interpretation Insight |
|---|---|
| Betaine | Low betaine with low choline suggests poor conversion and reduced methylation support. |
| SAM / SAH Ratio | Low ratio indicates slowed methylation due to insufficient methyl donors. |
| Homocysteine | Elevated levels confirm reduced choline- and betaine-dependent methylation efficiency. |
| Methionine | Low methionine suggests impaired homocysteine-to-methionine conversion. |
| Methylmalonic Acid (B12 Status) | Elevated values reflect B12 deficiency, worsening methylation inefficiency. |
| Liver Markers (e.g., Suberic Acid, Citrate) | May indicate mitochondrial stress or fatty liver related to low choline. |
This integrative view helps determine whether low choline results from dietary insufficiency, poor liver function, or increased methylation demand.
Clinical Implications of Low Choline
Persistently low choline levels can have widespread metabolic and neurological effects:
-
Cognitive decline and poor memory (low acetylcholine availability)
-
Fatty liver disease (NAFLD) due to reduced VLDL formation
-
Elevated homocysteine and cardiovascular risk
-
Low SAM and sluggish methylation
-
Hormonal imbalances and poor detoxification
-
Mitochondrial and redox dysfunction, contributing to fatigue
In pregnancy, low choline intake can impact fetal brain development, making adequate choline particularly important for maternal health.
Supportive Strategies to Discuss with Your Clinician
1. Increase Dietary Choline Intake
Include choline-rich foods such as:
-
Eggs (especially yolks)
-
Liver and fish (salmon, cod)
-
Chicken, turkey, and beef
-
Soybeans, legumes, quinoa, and cruciferous vegetables (for plant-based sources)
2. Optimize B-Vitamin Status
Ensure sufficient intake of:
-
Folate (5-MTHF)
-
Vitamin B12 (methylcobalamin)
-
Vitamin B6 (P5P)
-
Riboflavin (B2) and magnesium
These cofactors support choline’s methylation and homocysteine-lowering functions.
3. Support Liver Function and Detoxification
-
Include antioxidants (vitamin C, NAC, glutathione, alpha-lipoic acid) to protect against oxidative damage.
-
Avoid excessive alcohol or refined fats that tax hepatic methylation.
-
Consider liver-supportive botanicals like milk thistle, dandelion root, or artichoke extract under supervision.
4. Consider Choline Supplementation
If dietary intake is low or metabolic demand is high, choline supplementation may be beneficial.
Common forms include:
-
Alpha-GPC or Citicoline (CDP-Choline) — enhance brain acetylcholine and cognition
-
Phosphatidylcholine (lecithin form) — supports liver and cell membranes
-
Choline bitartrate — supports general methylation and liver function
Typical doses range from 250–1,000 mg/day, adjusted for dietary intake and clinical need.
5. Manage Inflammation and Oxidative Stress
Reduce lifestyle and environmental stressors that increase methylation demand, and ensure adequate antioxidant support to preserve choline-dependent pathways.
Key Takeaway
Choline is essential for healthy brain function, liver metabolism, and methylation balance. Low levels indicate reduced acetylcholine synthesis, weakened liver detoxification, and slowed methylation, often tied to poor diet, B-vitamin deficiency, or genetic inefficiency in methylation pathways.
On the Neurotransmitter XL panel, choline levels help reveal the body’s capacity to regulate neurotransmitter activity, lipid metabolism, and energy production.
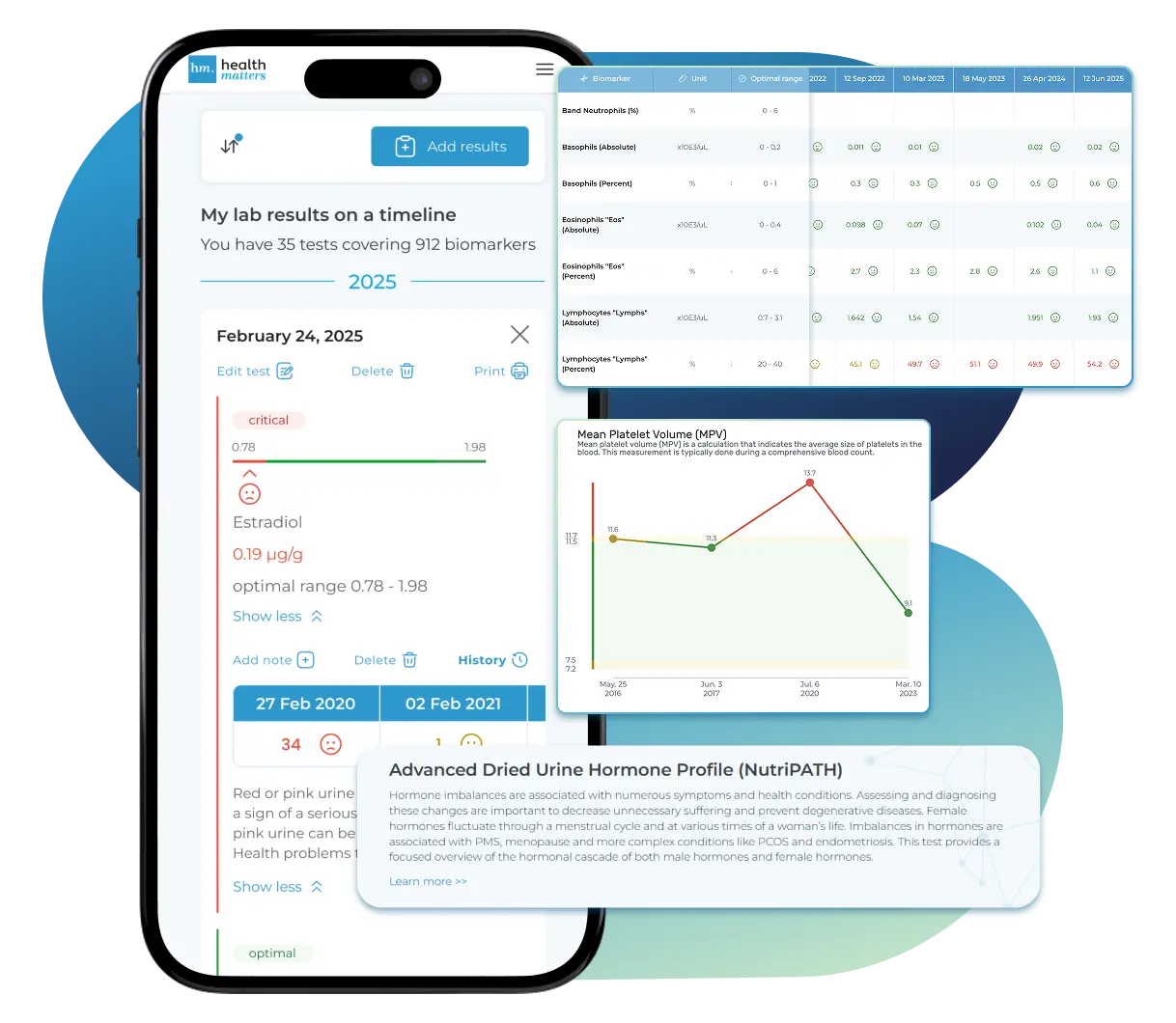
Lab Results Explained and Tracked
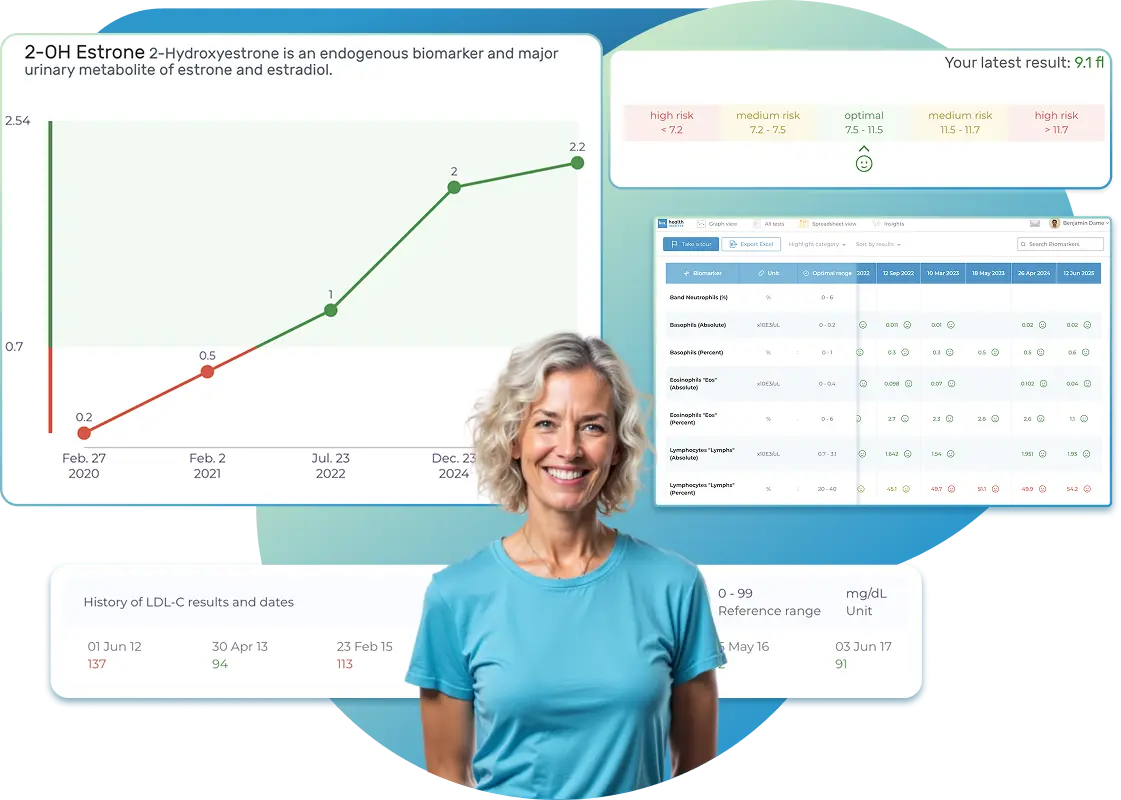
All Your Lab Results.
One Simple Dashboard.
Import, Track, and Share Your Lab Results Easily
Import, Track, and Share Your Lab Results
Import lab results from multiple providers, track changes over time, customize your reference ranges, and get clear explanations for each result. Everything is stored securely, exportable in one organized file, and shareable with your doctor—or anyone you choose.
Cancel or upgrade anytime
What does it mean if your Choline result is too low?
Low choline levels on the Neurotransmitter XL panel indicate a deficiency in one of the body’s most essential nutrients for neurotransmitter synthesis, liver function, and methylation balance. Choline serves as a building block for acetylcholine, the neurotransmitter responsible for memory, learning, attention, and muscle control, and is a critical precursor to phosphatidylcholine and betaine (trimethylglycine)—molecules central to cell membrane health, detoxification, and methyl group donation.
When choline is insufficient, the body’s ability to synthesize acetylcholine, maintain membrane integrity, and support the methionine cycle is compromised. This can manifest as fatigue, poor focus, low mood, and liver dysfunction, often accompanied by biochemical evidence of methylation slowdown, elevated homocysteine, or fat accumulation in the liver.
Low choline is particularly important to address early, as it often represents a foundational metabolic deficiency that disrupts both neurological performance and systemic detoxification.
Biochemical and Functional Implications
1. Reduced Acetylcholine Synthesis
Choline is converted into acetylcholine by the enzyme choline acetyltransferase, a reaction that underlies learning, memory retention, and neuromuscular coordination. When choline levels fall, acetylcholine production drops, leading to symptoms such as brain fog, memory lapses, poor focus, and low motivation.
2. Impaired Methylation and Homocysteine Recycling
Choline oxidation produces betaine, which donates methyl groups via the betaine-homocysteine methyltransferase (BHMT) pathway to regenerate methionine and sustain S-adenosylmethionine (SAM) production.
Low choline therefore weakens methylation efficiency, resulting in:
-
Elevated homocysteine levels (a marker of impaired methyl group recycling)
-
Reduced SAM, limiting neurotransmitter synthesis and detoxification
-
Sluggish catecholamine metabolism, causing stress intolerance or mood swings
3. Liver Fat Accumulation and Detoxification Impairment
Phosphatidylcholine, synthesized from choline, is essential for packaging and exporting fats from the liver as VLDL particles. Inadequate choline causes lipid buildup in hepatocytes, leading to fatty liver (hepatic steatosis) and reduced toxin elimination. This can result in sluggish digestion, poor fat tolerance, and hormonal imbalance due to decreased estrogen clearance.
4. Structural and Cellular Consequences
Choline is a major component of cell membranes. When levels are low, phospholipid synthesis is disrupted, compromising cell signaling, membrane fluidity, and mitochondrial protection. Over time, this can contribute to fatigue, oxidative stress, and reduced cellular repair capacity.
Causes of Low Choline
1. Inadequate Dietary Intake
The body’s choline requirement is high, and synthesis alone cannot meet demand. Diets low in eggs, fish, meat, and dairy—or strict vegan and vegetarian diets—often lead to choline insufficiency.
2. Increased Methylation Demand
Chronic stress, inflammation, toxin exposure, and high oxidative load accelerate methyl group turnover, depleting choline reserves faster than they can be replenished.
3. B-Vitamin Deficiency
Choline and B vitamins (B6, B12, folate) work synergistically in methylation. Deficiencies in these vitamins impair homocysteine conversion and SAM regeneration, increasing choline dependence.
4. Genetic Variants (PEMT, BHMT, MTHFR)
-
PEMT polymorphisms reduce phosphatidylcholine synthesis in the liver.
-
BHMT or MTHFR variants increase reliance on choline-derived methyl groups for homocysteine clearance.
Such genetic factors heighten the need for dietary or supplemental choline.
5. Liver Dysfunction or Malabsorption
Fatty liver, bile insufficiency, or gut dysbiosis can interfere with choline absorption and conversion to phosphatidylcholine, perpetuating deficiency.
Symptoms of Low Choline
Cognitive and Emotional Symptoms
-
Brain fog and forgetfulness
-
Poor concentration or low motivation
-
Mood swings or mild depression
-
Difficulty learning or processing information
-
Muscle fatigue or weakness (due to reduced acetylcholine)
Metabolic and Systemic Symptoms
-
Fatty liver or upper abdominal fullness
-
Elevated homocysteine
-
Hormonal imbalance (especially estrogen dominance)
-
Sensitivity to alcohol, caffeine, or medications
-
Low energy and oxidative stress symptoms
Low choline often appears together with low betaine and low SAM, reflecting a methylation system struggling to recycle homocysteine and maintain neurotransmitter balance.
Interpretation Context on Neurotransmitter XL
| Related Marker | Interpretation Insight |
|---|---|
| Betaine | Low choline with low betaine suggests reduced choline oxidation and methyl donor depletion. |
| SAM / SAH Ratio | A low ratio reflects insufficient methylation capacity due to inadequate choline-derived methyl groups. |
| Homocysteine | Often elevated when choline and betaine are low, indicating methylation inefficiency. |
| Methionine | Low methionine points to impaired homocysteine-to-methionine conversion. |
| Methylmalonic Acid (B12 Status) | Elevated levels further impair methylation, exacerbating choline demand. |
| Liver Stress Markers (e.g., Citrate, Suberic Acid) | Elevated values may indicate mitochondrial or hepatic overload due to low phosphatidylcholine synthesis. |
When interpreted in this biochemical context, low choline provides critical insight into how neurotransmitter, liver, and methylation pathways intersect under nutritional or metabolic strain.
Clinical Implications of Low Choline
Persistently low choline levels can lead to:
-
Cognitive decline and memory impairment (low acetylcholine)
-
Non-alcoholic fatty liver disease (NAFLD)
-
Elevated homocysteine and cardiovascular risk
-
Neurotransmitter imbalance (low dopamine and serotonin methylation)
-
Mood disorders, fatigue, and low stress resilience
-
Hormonal imbalance and sluggish detoxification
Because choline deficiency affects both neurological and systemic processes, addressing it can yield broad improvements in energy, cognition, and emotional stability.
Supportive Strategies to Discuss with Your Clinician
1. Increase Dietary Choline Intake
Focus on foods rich in choline:
-
Egg yolks (one of the richest sources)
-
Liver and fish (cod, salmon, sardines)
-
Chicken, turkey, and beef
-
Soy, lentils, quinoa, and cruciferous vegetables (for plant-based options)
2. Support with B-Vitamins and Methyl Donors
Optimize cofactors to reduce methylation stress:
-
Folate (5-MTHF), vitamin B12 (methylcobalamin), vitamin B6 (P5P)
-
Riboflavin (B2) and magnesium for enzyme activity
-
Betaine (TMG) or SAMe supplementation to enhance methylation efficiency
3. Strengthen Liver Function
-
Support phosphatidylcholine synthesis with lecithin or phosphatidylcholine supplements.
-
Use antioxidants (vitamin C, NAC, alpha-lipoic acid, glutathione) to protect hepatic cells.
-
Reduce alcohol, refined sugar, and processed fat intake to lessen liver strain.
4. Consider Choline Supplementation
Supplementation may be beneficial when dietary intake or conversion is insufficient.
Common forms:
-
Citicoline (CDP-Choline) – enhances brain acetylcholine and focus
-
Alpha-GPC – highly bioavailable, supports cognition and energy
-
Phosphatidylcholine (lecithin) – supports liver and cell membranes
Typical doses range from 250–1,000 mg/day, individualized to need.
5. Manage Inflammation and Oxidative Stress
Chronic oxidative burden accelerates choline depletion. Address inflammation through:
-
Omega-3 fatty acids (EPA/DHA)
-
Antioxidant support (CoQ10, NAC, vitamin E)
-
Stress management (sleep, mindfulness, moderate exercise)
Key Takeaway
Low choline levels indicate reduced acetylcholine synthesis, weakened methylation capacity, and impaired liver detoxification—a combination that can manifest as cognitive decline, fatigue, and metabolic imbalance.
On the Neurotransmitter XL panel, evaluating choline alongside betaine, SAM, homocysteine, and B-vitamin markers helps pinpoint whether the deficiency arises from nutritional insufficiency, genetic variants, or liver dysfunction.
Article Review & Sources
All our content is backed by peer-reviewed studies, academic research, and trusted medical sources. We're committed to accuracy and transparency — see our editorial policy for details.
Laboratories
Bring All Your Lab Results Together — In One Place
We accept reports from any lab, so you can easily collect and organize all your health information in one secure spot.
Pricing Table
Gather Your Lab History — and Finally Make Sense of It
Finally, Your Lab Results Organized and Clear
Personal plans
$79/ year
Advanced Plan
Access your lab reports, explanations, and tracking tools.
- Import lab results from any provider
- Track all results with visual tools
- Customize your reference ranges
- Export your full lab history anytime
- Share results securely with anyone
- Receive 5 reports entered for you
- Cancel or upgrade anytime
$250/ once
Unlimited Account
Pay once, access everything—no monthly fees, no limits.
- Import lab results from any provider
- Track all results with visual tools
- Customize your reference ranges
- Export your full lab history anytime
- Share results securely with anyone
- Receive 10 reports entered for you
- No subscriptions. No extra fees.
$45/ month
Pro Monthly
Designed for professionals managing their clients' lab reports
- Import lab results from any provider
- Track lab results for multiple clients
- Customize reference ranges per client
- Export lab histories and reports
- Begin with first report entered by us
- Cancel or upgrade anytime
About membership
What's included in a Healthmatters membership
 Import Lab Results from Any Source
Import Lab Results from Any Source
 See Your Health Timeline
See Your Health Timeline
 Understand What Your Results Mean
Understand What Your Results Mean
 Visualize Your Results
Visualize Your Results
 Data Entry Service for Your Reports
Data Entry Service for Your Reports
 Securely Share With Anyone You Trust
Securely Share With Anyone You Trust
Let Your Lab Results Tell the Full Story
Once your results are in one place, see the bigger picture — track trends over time, compare data side by side, export your full history, and share securely with anyone you trust.





Bring all your results together to compare, track progress, export your history, and share securely.
What Healthmatters Members Are Saying
We implement proven measures to keep your data safe.
At HealthMatters, we're committed to maintaining the security and confidentiality of your personal information. We've put industry-leading security standards in place to help protect against the loss, misuse, or alteration of the information under our control. We use procedural, physical, and electronic security methods designed to prevent unauthorized people from getting access to this information. Our internal code of conduct adds additional privacy protection. All data is backed up multiple times a day and encrypted using SSL certificates. See our Privacy Policy for more details.

















