Carcinoembryonic Antigen (CEA)
Other names: CEA (Carcino Embryonic Antigen), Serum
What Is CEA?
Carcinoembryonic Antigen (CEA) is a glycoprotein normally produced in high amounts during fetal development. After birth, levels fall to very low or undetectable concentrations in healthy adults.
CEA is classified as a tumor marker — a substance that may be elevated in the blood of individuals with certain cancers. It is most strongly associated with:
-
Colorectal cancer
-
Pancreatic cancer
-
Lung adenocarcinoma
-
Breast cancer
-
Gastric cancer
-
Medullary thyroid cancer (typically alongside calcitonin)
However, CEA is not cancer-specific and cannot diagnose cancer on its own.
Normal CEA Range
Reference ranges vary slightly by laboratory, but general guidelines are:
| Population | Typical Reference Range |
|---|---|
| Nonsmokers | 0 – 2.5 ng/mL |
| Smokers | 0 – 5.0 ng/mL |
Smoking can mildly elevate CEA even in the absence of disease. Many labs use higher cutoffs for smokers, but trends over time remain more important than absolute values.
What Does an Elevated CEA Mean?
CEA interpretation depends heavily on clinical context.
Mild Elevation (3–10 ng/mL)
May be seen in:
-
Early or localized cancer
-
Liver disease (cirrhosis, hepatitis, fatty liver)
-
Inflammatory bowel disease
-
Pancreatitis
-
COPD
-
Smoking
Repeat testing is usually recommended.
Moderate Elevation (10–20 ng/mL)
Increases the likelihood of malignancy, especially in someone with known cancer. Imaging studies are typically required.
High Elevation (>20 ng/mL)
More commonly associated with advanced or metastatic cancer — particularly colorectal cancer — but still requires confirmation through imaging and clinical evaluation.
Important: CEA cannot confirm cancer. It only signals that further investigation may be needed.
Why CEA Is Most Useful: Trend Monitoring
CEA is far more valuable when tracked over time.
-
The half-life of CEA is approximately 3–7 days
-
After complete tumor removal, levels typically normalize within 4–6 weeks
-
A consistent rise across multiple tests raises concern for recurrence
CEA monitoring can detect colorectal cancer recurrence 3–8 months before it becomes visible on imaging in some cases.
For this reason, storing and tracking results longitudinally is critical.
Primary Clinical Uses
1. Monitoring Colorectal Cancer
CEA is most commonly used for post-treatment surveillance in colorectal cancer.
Typical monitoring schedule:
-
Baseline before surgery
-
4–6 weeks after surgery
-
Every 3–6 months for the first 2 years
-
Every 6 months for years 3–5
A rising trend over 2–3 consecutive tests requires imaging.
Sensitivity for recurrence detection is approximately 60–80%, meaning not all recurrences produce elevated CEA.
2. Evaluating Treatment Response
-
Falling CEA during chemotherapy suggests treatment response
-
Stable or rising CEA may indicate treatment resistance or progression
-
Persistent elevation after surgery may suggest residual disease
3. Prognostic Indicator
In colorectal cancer, CEA >5 ng/mL at diagnosis is associated with:
-
Higher recurrence risk
-
More advanced disease stage
-
Worse overall prognosis
Normalization after surgery significantly improves outlook.
Non-Cancer Causes of Elevated CEA
CEA can be elevated in:
-
Liver disease (cirrhosis, hepatitis, fatty liver)
-
Inflammatory bowel disease
-
Pancreatitis
-
Chronic obstructive pulmonary disease (COPD)
-
Hypothyroidism
-
Smoking
-
Mild elevations during pregnancy (rare)
Because of these false positives, CEA is not recommended for cancer screening in asymptomatic individuals.
Limitations of the CEA Test
-
Not all cancers produce CEA
-
A normal CEA does not rule out cancer
-
Levels vary slightly between laboratories
-
CEA does not identify tumor location
-
Not appropriate for general cancer screening
It is most effective when combined with imaging (CT, MRI, PET) and clinical evaluation.
Low Value Interpretation
A low CEA level (within the reference range) generally indicates no active tumor marker elevation.
However:
-
Not all cancers produce CEA
-
Normal results do not rule out cancer
-
Continued monitoring may still be required in high-risk patients
Frequently Asked Questions
Can you have cancer with normal CEA?
Yes. Approximately 20–40% of colorectal cancers do not elevate CEA.
Can you have high CEA without cancer?
Yes. Smoking and several benign inflammatory or liver conditions can cause elevation.
What CEA level strongly suggests cancer?
There is no single diagnostic cutoff. Levels above 10 ng/mL increase suspicion, and levels above 20 ng/mL are more often associated with advanced disease — but diagnosis requires imaging or biopsy.
Should healthy individuals test CEA?
No. It is not recommended for screening.
Track Your CEA Results Over Time
CEA is most powerful when evaluated as a trend — not a single number.
With HealthMatters, you can:
-
Upload CEA results from multiple laboratories
-
View changes on a unified timeline
-
Compare CEA with other tumor markers (CA 19-9, CA 125, AFP, etc.)
-
Share organized reports securely with your oncologist
Monitoring patterns over months and years provides clearer insight than isolated lab values.
References
-
American Society of Clinical Oncology (ASCO) – Tumor Marker Guidelines
-
Cleveland Clinic – CEA Test Overview
-
StatPearls – Carcinoembryonic Antigen (2024)
-
MedlinePlus – CEA Blood Test
-
Colorectal Cancer Alliance – CEA Biomarker Guide
Lab Results Explained and Tracked
What does it mean if your Carcinoembryonic Antigen (CEA) result is too high?
An elevated CEA result does not have a single meaning. Interpretation depends on:
-
Whether cancer has already been diagnosed
-
Baseline CEA level
-
Smoking status
-
Liver health
-
Whether levels are rising or stable
Mild elevations
CEA levels between about 3–10 ng/mL can occur in both cancer and non-cancer conditions. Common non-cancer causes include:
-
Liver disease (fatty liver, hepatitis, cirrhosis)
-
Inflammatory bowel disease
-
Pancreatitis
-
Chronic lung disease
-
Smoking
These mild elevations often require repeat testing rather than immediate alarm.
Moderate to high elevations
Values above 10–20 ng/mL increase suspicion for malignancy, particularly in someone with a known cancer history. Levels above 20 ng/mL are more often associated with advanced disease, especially metastatic colorectal cancer, but still require imaging confirmation.
CEA alone cannot diagnose cancer or determine where it is located.
Why Trends Matter More Than Single Values
CEA has a half-life of approximately 3–7 days. After complete tumor removal, levels typically return to normal within 4–6 weeks. Because of this predictable behavior, changes over time provide meaningful information.
Patterns that may be clinically significant:
-
Rising CEA across multiple tests
-
Failure to normalize after surgery
-
Gradual increase after a period of stability
-
Sudden large increase
A single elevated result is rarely definitive. Serial measurements are far more informative.
Edge Cases: When CEA Is Flagged “High” but Only Slightly Elevated
One of the most common sources of confusion occurs when a CEA value is flagged as “high” even though it sits just above the laboratory reference range — for example:
Reference range: <2.5 ng/mL
Result: 2.5 ng/mL (flagged high)
This type of borderline elevation is extremely common and often not clinically significant on its own.
Why this happens
Laboratory reference ranges are statistical cutoffs, not absolute boundaries between health and disease. If the upper limit is 2.5 ng/mL, then a result of 2.5 or 2.6 may be flagged automatically even though the difference is minimal and within normal biological variation.
Factors that can cause small fluctuations:
-
Minor lab variability
-
Recent illness or inflammation
-
Smoking exposure
-
Liver enzyme changes
-
Normal day-to-day variation
-
Differences between laboratories
In many healthy individuals, CEA can fluctuate slightly around the upper reference limit without indicating disease.
How clinicians interpret borderline results
A value sitting just above the reference range is usually interpreted in context:
-
Has this person had cancer before?
-
Is the value rising over time?
-
Is there a baseline for comparison?
-
Are there liver or inflammatory conditions present?
If the value is stable and near the cutoff, most clinicians will:
-
Repeat the test in several weeks
-
Monitor trend over time
-
Avoid over-interpretation
What matters most is directional change, not a single borderline number.
When a borderline value matters more
A result near the upper limit becomes more meaningful if:
-
It is rising across multiple tests
-
There is a known cancer diagnosis
-
It was previously much lower
-
It continues increasing on repeat testing
Even then, clinicians rely on imaging and clinical evaluation rather than the CEA number alone.
Non-Cancer Causes of Elevated CEA
Many non-malignant conditions can increase CEA:
-
Liver disease
-
Inflammatory bowel disease
-
Pancreatitis
-
Chronic obstructive pulmonary disease
-
Smoking
-
Hypothyroidism
-
Certain infections
Because the liver helps clear CEA from the bloodstream, liver dysfunction is one of the most common reasons for mild elevation.
Limitations of the CEA Test
CEA is a valuable monitoring tool, but it has limitations:
-
Not all cancers produce CEA
-
A normal result does not rule out cancer
-
It cannot locate a tumor
-
It is not useful for general screening
-
Mild elevations are common and often benign
For these reasons, it is always interpreted alongside imaging, clinical history, and other laboratory tests.
What to Do if Your CEA Is Elevated
If your CEA is above the reference range:
-
Review whether you have a known cancer diagnosis
-
Compare with prior results
-
Consider repeat testing
-
Evaluate for non-cancer causes
-
Discuss with your physician
A single elevated value — especially a borderline one — rarely provides enough information on its own.
Tracking CEA Over Time
CEA is most informative when viewed as a timeline rather than a single data point. Watching how levels change over months and years can provide early insight into treatment response or recurrence risk.
Tracking results in one place allows for:
-
Clear visualization of trends
-
Comparison across laboratories
-
Integration with other tumor markers
-
Better communication with oncology teams
Longitudinal monitoring often provides more meaningful insight than any single result.
Summary
Carcinoembryonic Antigen is a widely used tumor marker for monitoring cancer, especially colorectal cancer. It is not a screening or diagnostic test. Mild elevations are common and often caused by non-cancer conditions, and values sitting just above the reference range frequently reflect normal variation rather than disease.
The most important factor in CEA interpretation is trend over time. A stable or borderline value near the upper limit is usually far less concerning than a steady upward pattern across multiple tests. Context, history, and longitudinal data are essential for accurate interpretation.
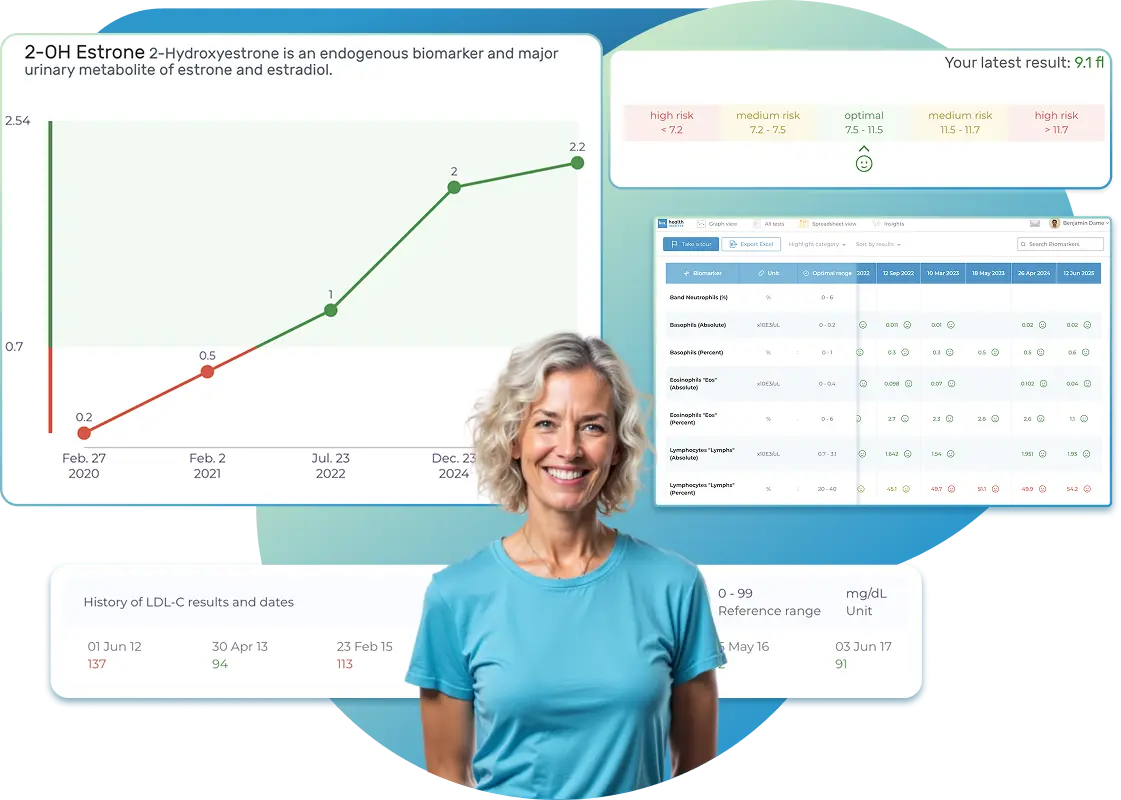
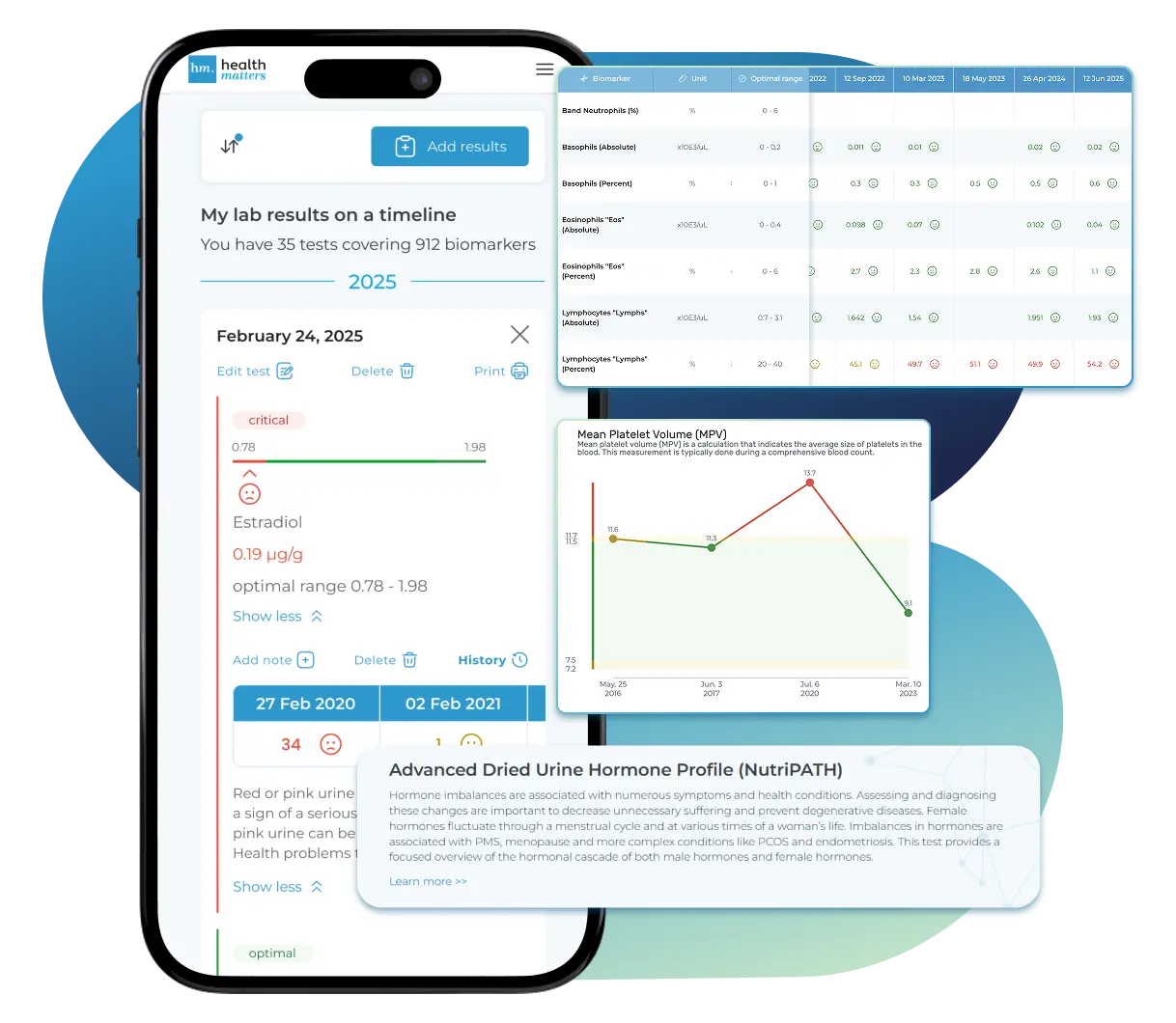
All Your Lab Results.
One Simple Dashboard.
Import, Track, and Share Your Lab Results Easily
Import, Track, and Share Your Lab Results
Import lab results from multiple providers, track changes over time, customize your reference ranges, and get clear explanations for each result. Everything is stored securely, exportable in one organized file, and shareable with your doctor—or anyone you choose.
Cancel or upgrade anytime
Article Review & Sources
All our content is backed by peer-reviewed studies, academic research, and trusted medical sources. We're committed to accuracy and transparency — see our editorial policy for details.
Laboratories
Bring All Your Lab Results Together — In One Place
We accept reports from any lab, so you can easily collect and organize all your health information in one secure spot.
Pricing Table
Gather Your Lab History — and Finally Make Sense of It
Finally, Your Lab Results Organized and Clear
Personal plans
$79/ year
Advanced Plan
Access your lab reports, explanations, and tracking tools.
- Import lab results from any provider
- Track all results with visual tools
- Customize your reference ranges
- Export your full lab history anytime
- Share results securely with anyone
- Receive 5 reports entered for you
- Cancel or upgrade anytime
$250/ once
Unlimited Account
Pay once, access everything—no monthly fees, no limits.
- Import lab results from any provider
- Track all results with visual tools
- Customize your reference ranges
- Export your full lab history anytime
- Share results securely with anyone
- Receive 10 reports entered for you
- No subscriptions. No extra fees.
$45/ month
Pro Monthly
Designed for professionals managing their clients' lab reports
- Import lab results from any provider
- Track lab results for multiple clients
- Customize reference ranges per client
- Export lab histories and reports
- Begin with first report entered by us
- Cancel or upgrade anytime
About membership
What's included in a Healthmatters membership
 Import Lab Results from Any Source
Import Lab Results from Any Source
 See Your Health Timeline
See Your Health Timeline
 Understand What Your Results Mean
Understand What Your Results Mean
 Visualize Your Results
Visualize Your Results
 Data Entry Service for Your Reports
Data Entry Service for Your Reports
 Securely Share With Anyone You Trust
Securely Share With Anyone You Trust
Let Your Lab Results Tell the Full Story
Once your results are in one place, see the bigger picture — track trends over time, compare data side by side, export your full history, and share securely with anyone you trust.





Bring all your results together to compare, track progress, export your history, and share securely.
What Healthmatters Members Are Saying
We implement proven measures to keep your data safe.
At HealthMatters, we're committed to maintaining the security and confidentiality of your personal information. We've put industry-leading security standards in place to help protect against the loss, misuse, or alteration of the information under our control. We use procedural, physical, and electronic security methods designed to prevent unauthorized people from getting access to this information. Our internal code of conduct adds additional privacy protection. All data is backed up multiple times a day and encrypted using SSL certificates. See our Privacy Policy for more details.

















